Research Projects
Ultrashort-pulsed laser skin treatment (超短パルスレーザーによる皮膚疾患治療)
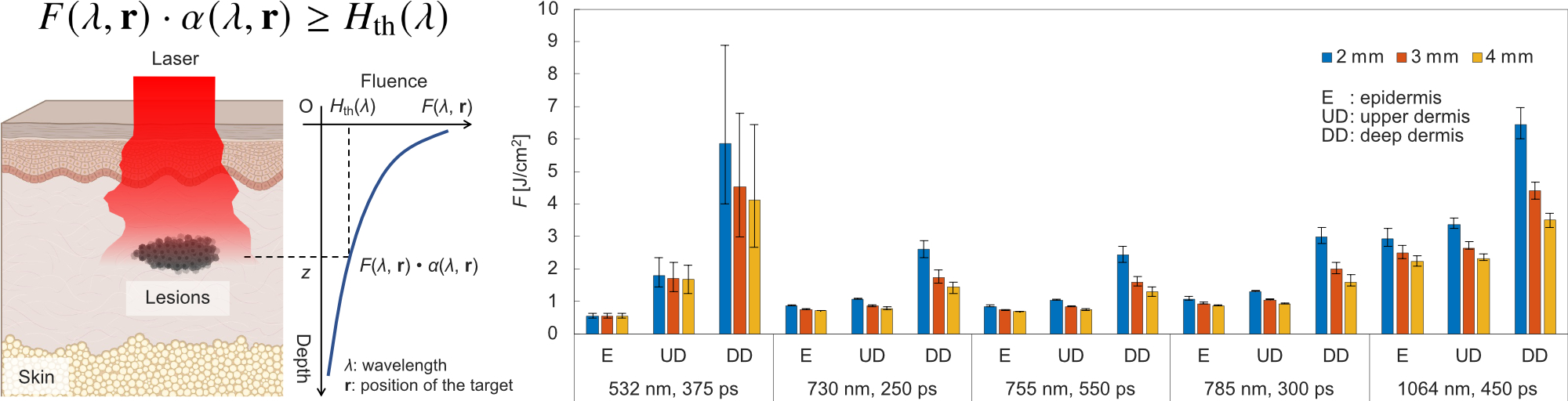
Pigmented skin lesions such as birthmarks and blemishes are caused by the excessive accumulation of melanin in certain areas of the skin. Laser therapy is the mainstream treatment. Among various types of lasers, picosecond lasers, which emit pulses in the range of one trillionth of a second, have recently gained considerable attention. Picosecond laser treatments have been reported to result in fewer complications, such as post-inflammatory hyperpigmentation and hypopigmentation. However, the laser parameters that most critically affect treatment outcomes are often determined based on the clinician’s experience, with no objective criteria currently available. This project aims to address this issue by elucidating picosecond laser-skin interactions and constructing a treatment model based on these findings. This enables the development of a technique to deliver highly reproducible and optimal laser treatment tailored to each patient’s unique skin characteristics and lesion properties.
アザやシミは、皮膚組織の一部にメラニン色素が過剰に沈着する症状です。 レーザー照射による治療が主流で、近年では1兆分の1秒の時間単位でレーザーを照射するピコ秒レーザーが注目されています。 ピコ秒レーザー治療では、炎症後色素沈着等の合併症が少ないと報告されていますが、治療効果に最も重要となる照射条件の設定は、術者の経験則に基づくことが多く、客観的な指標がありません。 本研究では、ピコ秒レーザーによる生体反応を解明し、それに基づく治療モデルを構築することで、一人ひとりの肌質や病変の状態に合わせて、最適な条件で再現性高くレーザー照射する技術を開発しています。
Related papers: Lasers Surg. Med. 57, 130-140 (2025) Lasers Surg. Med. 56, 404-418 (2024) Lasers Surg. Med. 53, 1096-1104 (2021)
In silico trial method (計算機臨床試験法)
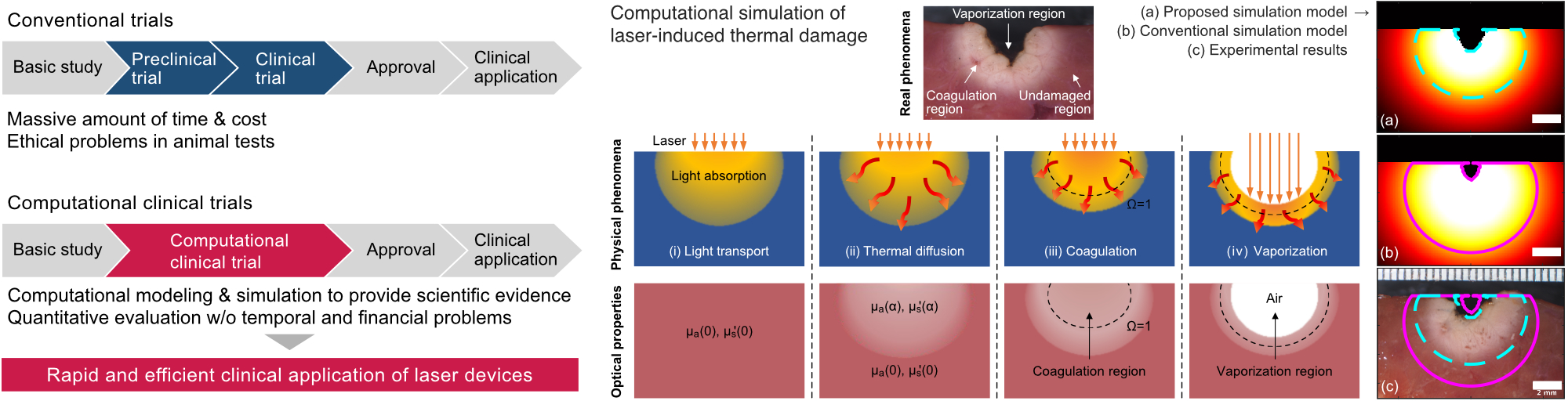
The advancement of optical devices for light and laser irradiation is crucial to expanding the clinical applications of optical diagnostics and therapeutic technologies. However, time and cost constraints associated with preclinical and clinical trials often hinder development. This project aims to overcome these challenges by developing computational modeling and simulation techniques that replicate the physicochemical reactions induced by laser irradiation in biological tissues. By virtually reproducing experiments traditionally conducted in the physical world, we are establishing a novel framework for in silico clinical trials. This approach is expected to complement and in some cases partially replace conventional preclinical and clinical testing. It offers a promising pathway to accelerate the clinical translation of new optical devices and contribute to the development of evidence-based clinical guidelines at reduced cost and time.
光診断・治療技術の臨床応用の拡大には、光・レーザーを照射する光学機器の高度化が重要ですが、臨床試験等にかかる時間・費用が制約となっています。 本研究では、レーザー照射によって生体組織に生じる物理化学反応のモデリング・計算機シミュレーション技術を開発し、これまで物理空間で行われていた試験を計算機上で再現する、計算機臨床試験という新たな試験法を開発しています。 これまでの前臨床試験・臨床試験を補完・一部代替することで、新規光学機器の迅速かつ低コストな臨床応用や診療ガイドラインの策定に貢献することが期待されます。
Related papers: JAAD Reviews 5, 82-90 (2025) Lasers Surg. Med. 55, 304-315 (2023) Laser Ther. 29, 61-72 (2020)
Development of minimally-invasive laser treatment technique (超低侵襲な疾患選択的レーザー治療技術の開発)
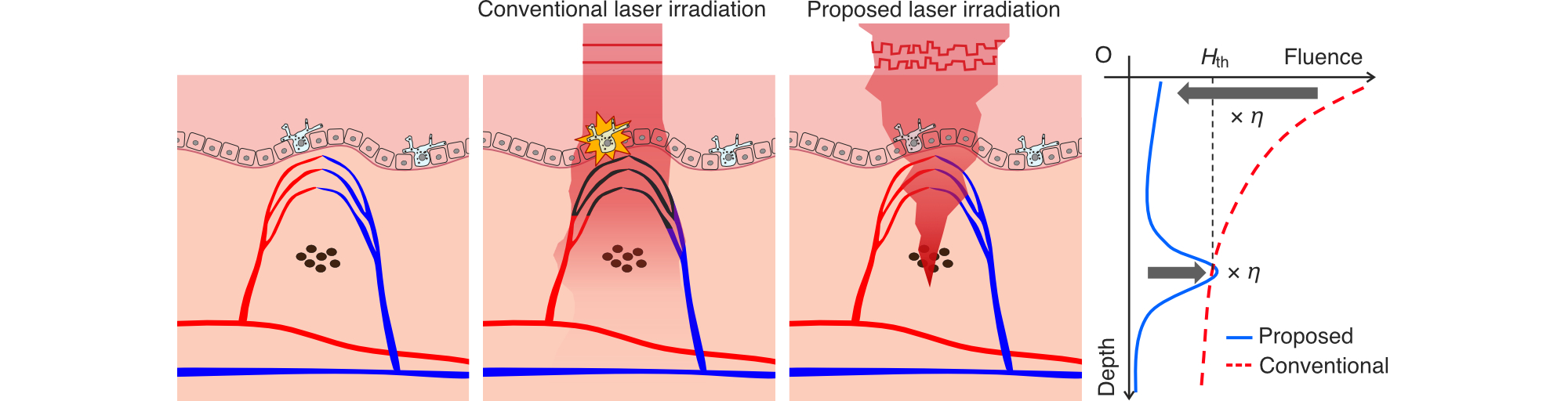
Lasers can be used to treat conditions such as pigmented lesions and cancers in a minimally invasive manner. However, as laser light scatters within biological tissues, some of the energy may be absorbed by non-target structures such as blood vessels or surrounding healthy tissue. Because therapeutic laser pulses carry extremely high energy, unintended absorption by normal tissue can lead to unwanted thermal injury and complications. This project focuses on developing laser technologies that enhance the selective delivery of laser energy to pathological targets while minimizing exposure to healthy tissue. By improving the lesion-specific biological responses to laser irradiation, we aim to establish safer, more precise, and non-invasive treatment methods.
レーザーは、シミ・あざ、がんを低侵襲に治療することができますが、レーザーが生体組織に散乱されて拡がることで、血管等の標的以外の正常組織に吸収されてしまいます。 治療で使用するレーザーのエネルギーは極めて高いため、正常組織に熱傷を誘発し合併症を生じる可能性があります。 本研究では、レーザーを標的に効率良く照射し、レーザーによる生体反応の病変選択性を向上させることで、正常組織に非侵襲な治療技術を開発しています。
Related papers: Sci. Rep. 14, 20112 (2024). Sci. Rep. 13, 2921 (2023).
Analysis of laser-tissue interactions (レーザー・光と生体組織との相互作用の解析)
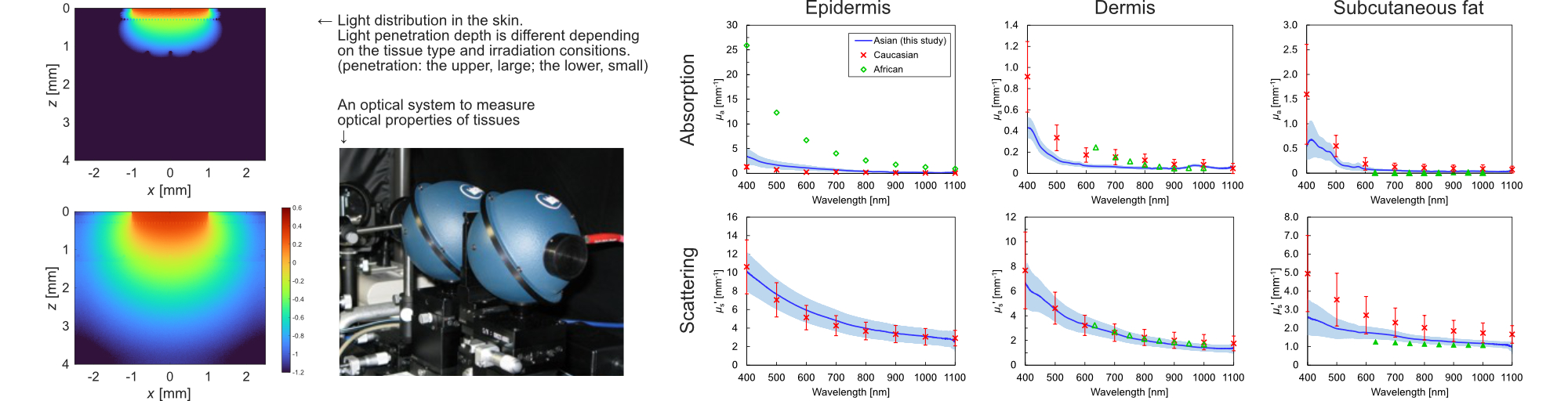
Optical diagnostics and therapeutic techniques are attractive for their non-invasive and minimally invasive nature. To ensure accurate and safe applications, it is essential to quantitatively understand how light propagates within biological tissues. The light distribution in tissue is primarily determined by the tissue’s optical properties, namely the absorption and reduced scattering coefficients. In this project, we are developing measurement systems and analysis algorithms to quantify these optical properties in various human and animal tissues. To date, we have measured and reported the optical properties of human lung, ureter, and renal pelvis tissues, as well as, for the first time globally, those of Asian human skin. We are currently compiling this data into a comprehensive optical property database. Furthermore, using the measured optical property data, we are constructing computational models that accurately calculate photothermal and photochemical effects induced by laser irradiation.
生体組織に対する非侵襲・低侵襲性が魅力である光診断・治療技術において、生体組織内の光分布を理解することは、 診断や治療している領域を定量的に把握し、正確かつ安全な診断・治療を実現するうえで非常に重要です。 組織内光分布は、生体組織の光学特性値(吸収係数、換算散乱係数)によって決まります。 本研究では、光学特性値を計測する測定システムや解析アルゴリズムを開発し、ヒトや動物の様々な組織を測定しています。 これまでにヒト肺、ヒト尿管・腎盂だけでなく、世界で初めてアジア地域のヒト皮膚の光学特性値も報告しており、現在はデータベース化を進めています。 さらに、測定した光学特性値を用いて、レーザー照射による光熱作用や光化学作用を正確に計算するシミュレーションモデルも開発しています。
Related papers: J. Biomed. Opt. 30, 048001 (2025) J. Biomed. Opt. 12, 125001 (2024) Sci. Rep. 13, 11898 (2023) J. Biomed. Opt. 25, 045002 (2020)
Photodynamic therapy for cancer and bacteria
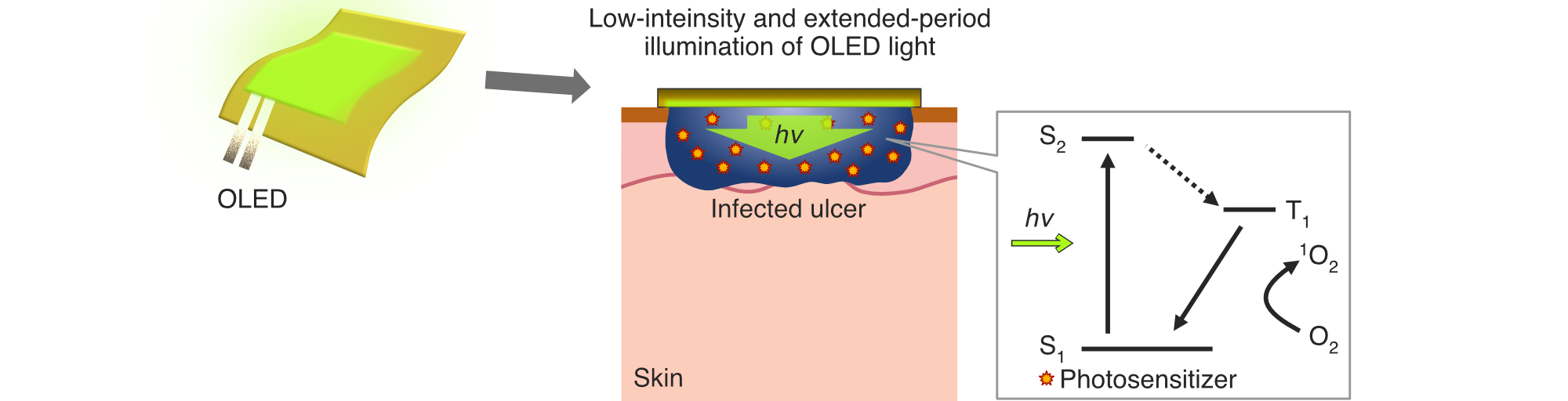
Photodynamic therapy (PDT) is a minimally invasive treatment that uses low-intensity light to activate photosensitizing agents selectively accumulated in target tissues. This activation generates reactive oxygen species, leading to anti-tumor or anti-microbial effects. This projet focuses on two key innovations to enhance the clinical utility of PDT. First, we are developing a home-based PDT system using flexible, wearable organic LED (OLED) films for the treatment of bacterial infections. Second, we are building a simulation platform for cancer PDT that enables precise light delivery, based on experimentally measured optical properties of normal and tumor tissues. These approaches aim to expand access to PDT and improve its therapeutic precision.
光線力学治療 (Photodynamic therapy; PDT) は、標的に蓄積させた光感受性薬剤へ低強度の光を照射し、活性酸素種を生成させることで抗腫瘍効果・殺菌効果をもたらす低侵襲な治療法です。 本研究では、在宅治療に向けた、貼付け式の有機ELフィルムを用いた細菌PDTの開発や、がんPDTの光照射管理に向けた、正常組織と腫瘍組織の実測した光学特性値に基づく治療シミュレータを開発しています。
Related papers: Photodermatol. Photoimmunol. Photomed. 40, e12959 (2024) JJSLSM 45, 153-160 (2024)